Covid-19 Moms Are at Higher Risk for ICU Admission and Complications
An OB-GYN reviews the latest coronavirus research in pregnancy.
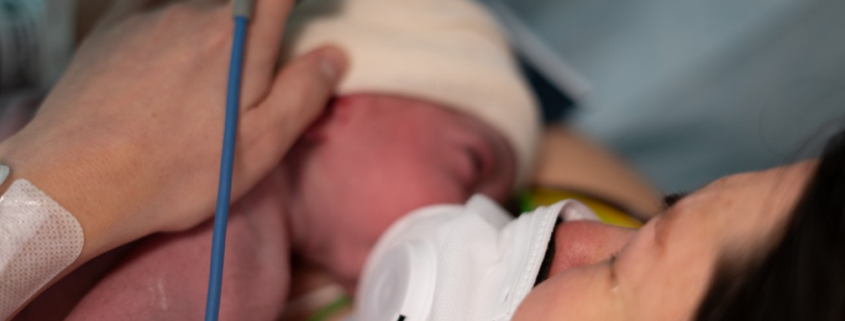
No pregnant woman wants to give birth during a pandemic. Obstetricians worldwide work to protect our patients and keep them safe. Scientists continue to learn more about the novel coronavirus’s effects on pregnant women and babies, but much remains unknown.
The U.S. Centers for Disease Control and Prevention (CDC) provides updated guidance for public health information and recommendations through the weekly Morbidity and Mortality Weekly Report (MMWR). On November 2, the CDC released a report on pregnant women’s maternal outcomes who contract Covid-19.
The report, titled Characteristics of Symptomatic Women of Reproductive Age with Laboratory-Confirmed SARS-CoV-2 Infection by Pregnancy Status, evaluated symptomatic women aged 15–44 with laboratory-confirmed infection with SARS-CoV-2.
This paper verifies the growing scientific consensus that women are at a higher risk of severe complications if they acquire Covid-19 during pregnancy compared with nonpregnant women. The analysis of approximately 400,000 women with symptomatic Covid-19 infections had a low overall risk of serious complications. Still, pregnancy increased the risk of intensive care unit admission, invasive ventilation, extracorporeal membrane oxygenation (ECMO), and death.
Based on current data, there is no evidence at this time indicating pregnant women are more at risk for severe illness from Covid-19 than the general public. We know that viral infections in pregnancy and postpartum can lead to poor outcomes in mothers and newborns.
Pregnant women have a suppressed immune system and physiologic changes in their lung function. These changes put pregnant women at a higher risk for respiratory problems when they contract other similar viruses, such as MERS, SARS, influenza, or pneumonia.
On the plus side, data so far indicates that a Covid-19-positive pregnant woman has a low risk of passing the virus to her baby. The PRIORITY study (Pregnancy Coronavirus Outcomes Registry) showed babies born to Covid-19 positive women do well with no increase in important metrics such as low birth weight, difficulty breathing, apnea, or respiratory infections through the first eight weeks of life. The PRIORITY study showed that only 1.1% of infants contract the virus.
A November 6 CDC paper titled Birth and Infant Outcomes Following Laboratory-Confirmed SARS-CoV-2 Infection in Pregnancy demonstrated that pregnant women are at a higher risk of preterm labor if they acquire Covid-19 during pregnancy.
Although the increased risk of preterm labor is problematic, the low rate of infant transmission is encouraging. Yet obstetricians and pregnant women need more information revealing how moms do when they contract Covid-19.
This MMWR report sheds some light on this topic. Pregnancy data was collected through the National Notifiable Diseases Surveillance System (NNDSS) and reported to the CDC. Health history data was analyzed from 23,434 symptomatic pregnant patients from January to October. Asymptomatic carriers of SARS-CoV-2 were excluded from this analysis.
Most Covid-19-positive moms do well
The data showed symptomatic pregnant women with Covid-19 had a low overall risk of complications. This finding is important for health care providers, pregnant patients, and their families.
Most symptomatic Covid-19-positive moms do not experience severe disease. For example, ICU admission rates were 10.5/1,000 cases, invasive ventilation 2.9/1,000 cases, and death 1.5/1,000 cases.
Overall, most pregnant women experience mild symptoms and do not require hospitalization.
Covid-19-positive moms are at higher risk than nonpregnant women
Importantly, this study demonstrates pregnant women who contract SARS-CoV-2 do not fare as well as nonpregnant women of the same age group. Covid-19-positive pregnant women were more likely to be admitted to the intensive care unit, nearly four times more likely to need invasive ventilation, and twice as likely to die.
Even after adjusting for age, race, and preexisting medical conditions, the severe disease and respiratory compromise risk were present in all age groups.
ICU admission risk was higher among all pregnant women but highest among Asian and Native Hawaiian/Pacific Islander women. Among Latinas, Covid-19-positive pregnant women had 2.4 times the risk of death.
The study mentions an interesting and unexplained finding that pregnant women reported symptoms less often than nonpregnant women. The most common symptoms mentioned by pregnant and nonpregnant women were cough, headache, muscle aches, and fever.
Limitations of the study
The authors report limitations to this important publication. There is not a national standard for reporting data. National case surveillance data for Covid-19 is reported voluntarily by health care providers and public health agencies.
Case reporting varies by jurisdiction. Race and ethnicity were missing in 25% of reported cases. Symptoms and preexisting condition data were missing in approximately 50% of cases.
This study was limited to symptomatic patients with known pregnancy status, but in 64.5 % of reported Covid-19 cases, the pregnancy status was not reported.
How does this report help doctors manage pregnancy?
This CDC report adds essential information to the growing scientific literature to help health care providers manage pregnant women with Covid-19.
We can reassure women and families that the overall risk of severe complications from Covid-19 is low, but pregnant women should be counseled that their risk for severe Covid-19-associated illness is higher than that of nonpregnant women.
Health care providers should take extra caution, knowing that when a pregnant woman is symptomatic with Covid-19 she is more likely than nonpregnant women to experience respiratory distress and require ICU admission.
How do pregnant women protect themselves from Covid-19?
We all must do our part to prevent the spread of the virus. Pregnant women should follow the same global recommendations:
- Wash your hands with soap and water for at least 20 seconds.
- Use hand sanitizer containing at least 60% alcohol.
- Avoid touching your face.
- Practice social distancing.
- Cover your mouth if you cough or sneeze.
- Clean your cellphone and household surfaces.
- Avoid travel.
- Wear a mask when out in public.
CDC Morbidity and Mortality Weekly Report, “Update: Characteristics of Symptomatic Women of Reproductive Age with Laboratory-Confirmed SARS-CoV-2 Infection by Pregnancy Status — United States, January 22–October 3, 2020.”
Thank you Medium Coronavirus Blog for publishing this article on Medium.
Blog Author: Dr. Jeff Livingston
Main Blog Photo By: Dario Sintoni iStock by Getty